
In the city of Camden, New Jersey, a pioneering healthcare initiative is demonstrating that the path to stabilizing chronic illness often begins far outside the walls of a traditional doctor’s office. The Healthy Neighbor program, a collaborative effort led by the regional healthcare provider Virtua Health in partnership with global medical technology leader Medtronic and its social enterprise arm, Medtronic LABS, is fundamentally altering the trajectory of patient outcomes by treating the social environment as a critical component of clinical care. By deploying community health workers (CHWs) directly into the homes of residents struggling with type 2 diabetes and hypertension, the program is bridging a long-standing gap in the American healthcare system—the divide between medical intervention and the daily realities of poverty, housing instability, and food insecurity.
The Camden Health Crisis and the Necessity of Intervention
The impetus for the Healthy Neighbor program lies in the stark health disparities that define the Camden metropolitan area. While the city is located just miles from some of the most affluent suburbs in the United States, its residents face a drastically different reality. Statistical data indicates that Camden residents live up to 16 years less than individuals residing just six miles away. This life expectancy gap is not a result of a lack of medical facilities—Camden is home to a robust "eds and meds" corridor—but rather a consequence of systemic social determinants of health (SDOH).
Social determinants of health are the conditions in which people are born, grow, live, work, and age. According to the World Health Organization (WHO), these factors are responsible for between 30% and 55% of health outcomes. In Camden, a city of approximately 70,000 people where the poverty rate consistently hovers significantly above the national average, these determinants manifest as "food deserts," substandard housing, and high levels of toxic stress. For a patient with type 2 diabetes, the ability to manage blood sugar is often secondary to the immediate need for safe shelter or the struggle to afford fresh produce over processed, shelf-stable goods.
A Longitudinal Model of Trust and Technology
The Healthy Neighbor program differentiates itself from traditional outreach by its duration and the depth of the relationship between the provider and the patient. Rather than a one-time consultation, the program offers a 12-month intervention. This timeline is intentional, designed to move past the "crisis management" phase of healthcare and into sustainable lifestyle transformation.
The process typically begins with a clinical trigger, such as an emergency room visit or a hospital admission. For many participants, like a resident named Charmaine, the hospital serves as the point of entry into a system that finally looks at the "whole person." After being identified as eligible based on her diagnosis of type 2 diabetes and chronic obstructive pulmonary disease (COPD), Charmaine was paired with Fanny Ochoa, a community health worker.
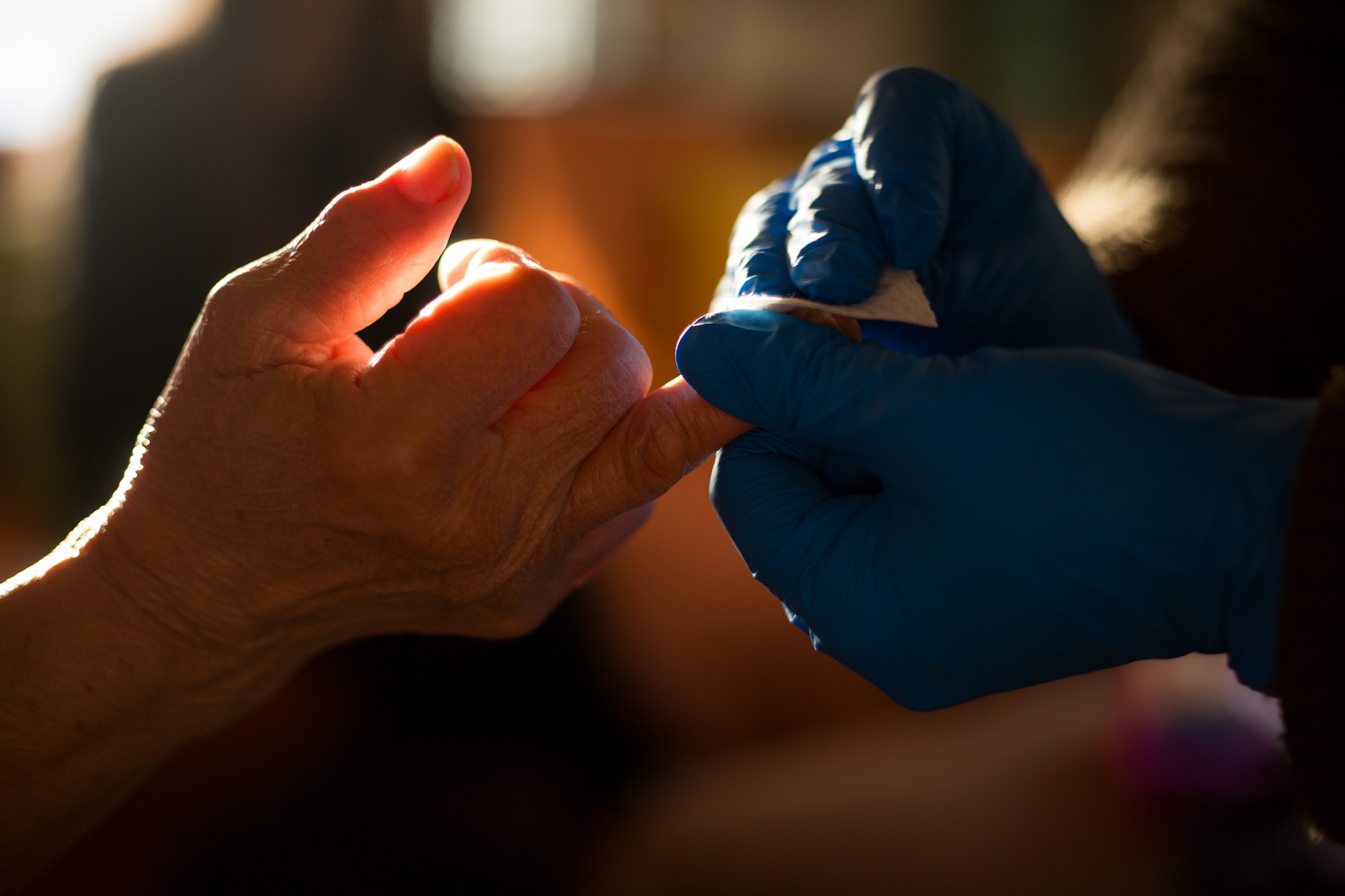
The role of the CHW is multifaceted. They are not doctors or nurses, but they are trained professionals who often come from the same communities they serve, allowing them to build a level of trust that traditional clinicians may struggle to achieve. During monthly home visits, CHWs like Ochoa perform clinical tasks—such as testing blood sugar via lancets and monitoring blood pressure—while simultaneously conducting social assessments. This dual approach allowed Ochoa to identify that Charmaine’s health was being exacerbated by the profound grief of losing two sons and the lack of stable, affordable housing.
Integrating Clinical Data with Social Solutions
To support the clinical side of the intervention, the program leverages advanced medical technology provided by Medtronic LABS. Participants are often equipped with continuous glucose monitors (CGMs)—tiny wearable sensors that provide real-time data on blood sugar levels. This technology allows patients to see the immediate impact of their diet and activity on their health, turning abstract medical advice into tangible, actionable data.

However, data alone cannot fix a broken environment. The Healthy Neighbor program acts as a central hub, connecting patients to a network of local resources. When a CHW identifies food insecurity, the patient is referred to Virtua Health’s "Eat Well" program. This initiative includes a "Food Farmacy" and mobile grocery stores that deliver fresh fruits and vegetables to underserved neighborhoods. Patients can use "food bucks" provided by the program, Supplemental Nutrition Assistance Program (SNAP) benefits, or traditional payment methods to access nutrition that is otherwise unavailable in their immediate vicinity.
Housing is addressed with equal urgency. The program collaborates with organizations like the Michaels Organization to place patients in developments like Oliver Station. This specific affordable housing solution in Camden includes on-site primary care, effectively embedding the healthcare system into the patient’s living environment. For patients like Denise, another program participant who was previously living in a condemned building while attempting to manage uncontrolled hypertension, this transition to safe housing was the primary driver of her eventual clinical stabilization.
Quantifiable Success: Data and Outcomes
The effectiveness of the Healthy Neighbor model is reflected in the clinical data collected over its operational period. According to Virtua Health, the program has achieved the following results:
- Hypertension Control: 74% of patients with previously uncontrolled hypertension saw a meaningful and sustained improvement in their blood pressure readings.
- Diabetes Management: Nearly 70% of type 2 diabetic patients experienced a significant drop in their HbA1c levels, a key indicator of long-term blood sugar control.
- Reduced Readmissions: By addressing the root causes of health crises at home, the program aims to reduce the "revolving door" of emergency room visits, which places a heavy financial burden on the broader healthcare system.
These metrics suggest that when the barriers to health—such as the inability to store insulin in a refrigerator due to lack of electricity or the inability to exercise in an unsafe neighborhood—are removed, patients are highly capable of managing their own chronic conditions.

Strategic Expansion and the "Toolkit" for National Replication
Recognizing that the challenges faced in Camden are mirrored in urban and rural centers across the United States, Virtua Health and Medtronic LABS have taken steps to "open source" their methodology. In August 2025, the organizations released a comprehensive toolkit designed to help other hospital systems and municipalities replicate the Healthy Neighbor model.
The toolkit provides a roadmap for building a CHW team, integrating social service referrals into clinical workflows, and utilizing data platforms to track patient progress. Daniel Master, the director of community health and impact at Virtua Health, emphasized that the goal is to create a sustainable framework that survives beyond the initial intervention period. "We know that our intervention is up to 12 months, and a lot is going to happen after that year," Master stated. "We bring all of those resources to patients so that their care can be sustainable."
The program is currently expanding within Camden, supported by a grant from the city government. This funding allows for the hiring of additional community health workers, increasing the program’s capacity to serve a larger segment of the population.
Policy Implications and the Future of Reimbursement
Despite the clear clinical and social benefits, the expansion of programs like Healthy Neighbor faces significant structural hurdles, most notably in the realm of insurance and reimbursement. Currently, the American insurance landscape is largely fee-for-service, meaning providers are paid for specific medical procedures rather than for the long-term "wellness" of a patient.

Community health workers, despite their efficacy, often lack a reliable reimbursement mechanism. Unlike a registered dietitian or a physical therapist, CHW services are frequently not covered by private insurers or Medicaid in a consistent manner. Master pointed out that this lack of a funding stream is a primary barrier to scaling the model nationwide. For the Healthy Neighbor program to become a standard of care, policy changes are required at the state and federal levels to recognize CHWs as essential members of the healthcare team whose work justifies financial coverage.
Conclusion: A New Paradigm for Public Health
The Healthy Neighbor program represents a shift away from the reactive nature of modern medicine toward a proactive, holistic model of public health. By acknowledging that a prescription for medication is useless if a patient cannot afford the food required to take it, or the bus fare to pick it up, Virtua Health and Medtronic are challenging the healthcare industry to broaden its definition of "treatment."
The success stories of residents like Charmaine and Denise serve as a proof of concept. When healthcare providers step out of the clinic and into the community, they do more than just treat a disease; they restore agency and dignity to individuals who have long been marginalized by the system. As the program looks toward future expansion, it stands as a testament to the power of trust, technology, and the recognition that a person’s zip code should not be the primary determinant of their lifespan.






