
In the city of Camden, New Jersey, a revolutionary approach to public health is demonstrating that the path to clinical recovery often begins far outside the walls of a doctor’s office. The Healthy Neighbor program, a collaborative initiative led by the regional healthcare provider Virtua Health in partnership with global medical technology leader Medtronic and its social enterprise arm, Medtronic LABS, is redefining the parameters of chronic disease management. By integrating social determinants of health—such as housing stability, nutritional access, and emotional support—directly into the clinical treatment plan, the program is achieving measurable improvements in patients suffering from type 2 diabetes and hypertension, two of the most persistent health challenges in underserved urban environments.
The program’s philosophy is rooted in the recognition that medical prescriptions are often ineffective if the patient lacks a stable environment in which to follow them. In Camden, a city of approximately 70,000 residents, the urgency of this intervention is underscored by a startling statistic: residents of certain Camden neighborhoods live up to 16 years less than those residing just six miles away in more affluent suburbs. This life expectancy gap is not merely a product of genetics or personal choice but is driven by systemic poverty, environmental stressors, and a lack of access to the fundamental resources required for a healthy life.
The Human Face of Holistic Intervention
The efficacy of the Healthy Neighbor program is best illustrated through the lived experiences of its participants. For Charmaine, a Camden resident who had recently endured the devastating loss of two sons while struggling with type 2 diabetes and chronic obstructive pulmonary disease (COPD), a routine hospital visit served as the catalyst for a life-altering intervention. Upon her discharge, the hospital alerted the Healthy Neighbor team, triggering a transition from reactive emergency care to proactive community-based support.
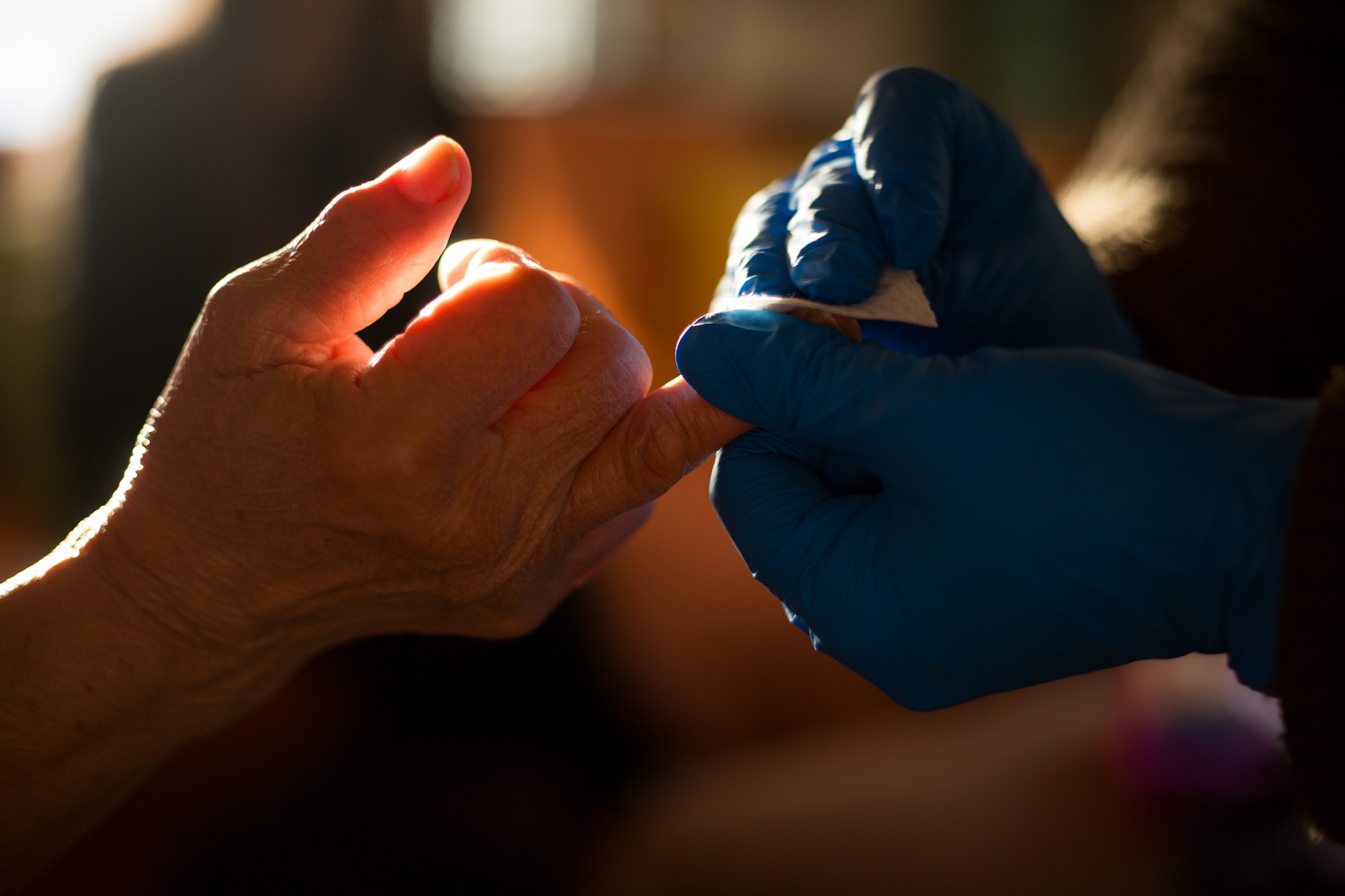
Fanny Ochoa, a community health worker (CHW) with the program, began visiting Charmaine in her home, establishing a relationship built on trust rather than clinical coldness. Ochoa’s assessment went beyond blood sugar readings; she identified that Charmaine’s physical health was inextricably linked to her housing insecurity and profound grief. Over the course of a year, the two worked as a team. Ochoa facilitated Charmaine’s move into Oliver Station—a modern, affordable housing development in Camden created by the Michaels Organization and Virtua Health—which features on-site primary care. With the burden of housing removed and consistent mental health support provided, Charmaine’s clinical markers followed suit. Today, her COPD is managed, and her blood sugar levels are within a healthy range.
Similarly, La Shawn Dutton-Spruill, another community health worker on the team, recounts the transformation of a patient named Denise. When Denise first entered the program, she was living in a condemned building, skipping vital medications, and suffering from uncontrolled hypertension and diabetes. The program did not simply hand her a new prescription; it addressed the "food-impacted" nature of her condition. By connecting Denise with Virtua Health’s "Eat Well" program—which provides fresh produce and groceries through mobile markets and "Food Farmacies"—the Healthy Neighbor initiative ensured she had the nutritional foundation to support her medication. Denise has since transitioned to safe housing and reports a significant reduction in depressive symptoms, illustrating the program’s ability to "turn a life around" by addressing the root causes of instability.
A Chronology of Care: From Hospital to Home
The Healthy Neighbor program operates on a structured timeline designed to foster long-term behavioral change and physiological stabilization. The process typically begins with a referral, often following a patient’s encounter with the acute care system. Once enrolled, the patient is paired with a community health worker for a period of up to 12 months.
- Initial Assessment (Months 1-2): CHWs conduct comprehensive home visits to evaluate the patient’s clinical vitals (blood pressure and glucose) alongside their social needs. This includes auditing the patient’s pantry, assessing the safety of their living environment, and identifying barriers to transportation or medication adherence.
- Goal Setting and Resource Integration (Months 3-6): The CHW and patient establish collaborative goals. If food insecurity is identified, the patient is enrolled in the Eat Well program, which allows them to use federal Supplemental Nutrition Assistance Program (SNAP) benefits or "food bucks" provided by the program to purchase fresh produce. If housing is the primary barrier, the team coordinates with local nonprofits and developers.
- Technological Monitoring (Ongoing): Leveraging Medtronic’s technological expertise, patients are often equipped with wearable sensors, such as continuous glucose monitors (CGMs), which provide real-time data to both the patient and the healthcare team. This technology empowers patients to see the immediate impact of diet and activity on their health.
- Sustainability and Graduation (Months 10-12): The final phase of the program focuses on ensuring the patient can maintain their health independently. This involves finalizing permanent housing solutions and ensuring the patient is comfortable navigating the primary care system without the daily oversight of a CHW.
Quantifying Success: Data-Driven Results
The Healthy Neighbor program is not merely a feel-good social initiative; it is a data-backed clinical success. According to internal metrics released by Virtua Health, the program has achieved remarkable outcomes in a population that has traditionally been difficult for the healthcare system to reach effectively.

Data indicates that 74 percent of patients who entered the program with uncontrolled hypertension saw a meaningful and sustained improvement in their blood pressure readings. Furthermore, nearly 70 percent of patients with type 2 diabetes experienced a significant drop in their A1C (blood sugar) levels. These improvements are particularly notable because they were achieved in a demographic that often faces "falling through the cracks" of traditional, office-based medical models.
The program’s success is attributed to its "one model" approach, which addresses clinical and social factors simultaneously. By leveraging the resources of a large health system like Virtua and the technological infrastructure of Medtronic LABS, the initiative provides a level of wrap-around care that smaller community clinics often cannot afford to sustain.
Official Responses and the Push for Scalability
Daniel Master, the Director of Community Health and Impact at Virtua Health, emphasizes that the program’s uniqueness lies in its integration. "If a patient is currently experiencing homelessness, before we can even talk about reducing their blood sugar levels or hypertension, we need to figure out how to get them to a better and more reliable housing situation," Master stated. He noted that once the housing and food barriers are removed, "measurable clinical improvements" almost always follow.
Recognizing the potential for this model to serve as a national blueprint, Virtua Health and Medtronic LABS have released a comprehensive toolkit. This "open source" guide is intended to help other hospital systems across the United States replicate the Camden model. The initiative has also received tangible support from the local government; a grant from the City of Camden has allowed the program to expand its team of community health workers to reach a broader segment of the population.

However, the path to national expansion faces significant hurdles, primarily regarding financial sustainability. Master pointed out a critical gap in the current American healthcare landscape: the lack of a reliable reimbursement mechanism for community health workers. While insurance providers typically cover the costs of nutritionists, educators, and physicians, the "boots-on-the-ground" work of CHWs—who navigate the complexities of social services and home visits—often lacks a dedicated funding stream from insurers.
Broader Implications for the Future of Healthcare
The Healthy Neighbor program arrives at a time when the U.S. healthcare industry is increasingly grappling with the limitations of the traditional fee-for-service model. The Camden initiative suggests that a "value-based" care model, which rewards outcomes rather than the volume of procedures, must include social interventions to be truly effective.
The implications of this program extend beyond individual health. By stabilizing patients in their homes and reducing their reliance on emergency rooms for chronic disease management, programs like Healthy Neighbor have the potential to significantly reduce the overall cost of care for the public health system. Emergency department visits and hospital readmissions for preventable complications of diabetes and hypertension are among the highest drivers of healthcare spending in the United States.
As Virtua Health looks toward expanding the program beyond Camden’s borders, the focus remains on the intersection of healthcare, government, and the social service sector. The success in Camden serves as a powerful argument for a more integrated societal approach to wellness. In the words of Daniel Master, "Housing, financial challenges, and healthy food access will continue to be a perennial issue for communities. We believe we are paving the way for what that could look like."

For the residents of Camden, the program represents more than just a medical intervention; it is a restoration of agency. For patients like Denise and Charmaine, the transition from surviving in a state of chronic crisis to "living life to the fullest" is the ultimate metric of success. As the healthcare industry watches the Camden experiment, the Healthy Neighbor program stands as a testament to the idea that in the fight against chronic disease, a neighborly hand can be just as vital as a doctor’s prescription.






