
In the city of Camden, New Jersey, a pioneering community-based healthcare model is demonstrating that the key to managing chronic illness lies far beyond the walls of a traditional doctor’s office. The Healthy Neighbor program, a collaborative effort led by Virtua Health and supported by global medical technology leader Medtronic and Medtronic LABS, is transforming patient outcomes by treating social and environmental factors—such as housing instability and food insecurity—as integral components of medical treatment. By deploying community health workers (CHWs) directly into the homes of high-risk residents, the initiative is closing a staggering 16-year life expectancy gap that exists between Camden and its more affluent neighbors just six miles away.
The Socioeconomic Landscape of Health in Camden
Camden, a city of approximately 70,000 residents, has long grappled with systemic poverty and industrial decline, factors that have created a profound public health crisis. Statistical data reveals that a resident’s zip code is often a more accurate predictor of their health outcomes than their genetic code. In Camden, many individuals face "food-impacted" chronic conditions, where the inability to access fresh, nutritious produce exacerbates diseases like Type 2 diabetes and hypertension.
The Healthy Neighbor program was established to address these disparities head-on. Unlike traditional medical interventions that focus solely on pharmaceutical compliance, this model recognizes that a patient cannot prioritize blood sugar management if they are living in a condemned building or grieving the loss of family members without emotional support. The program targets adults with uncontrolled chronic conditions, providing them with a dedicated community health worker for a duration of up to one year.
A Personalized Approach to Chronic Disease Management
The efficacy of the Healthy Neighbor model is best illustrated through the lived experiences of its participants. For Charmaine, a Camden resident struggling with Type 2 diabetes and chronic obstructive pulmonary disease (COPD), the program served as a lifeline following the tragic loss of two sons. Her journey began not in a clinic, but in a hospital bed, where she was identified as a candidate for the program.
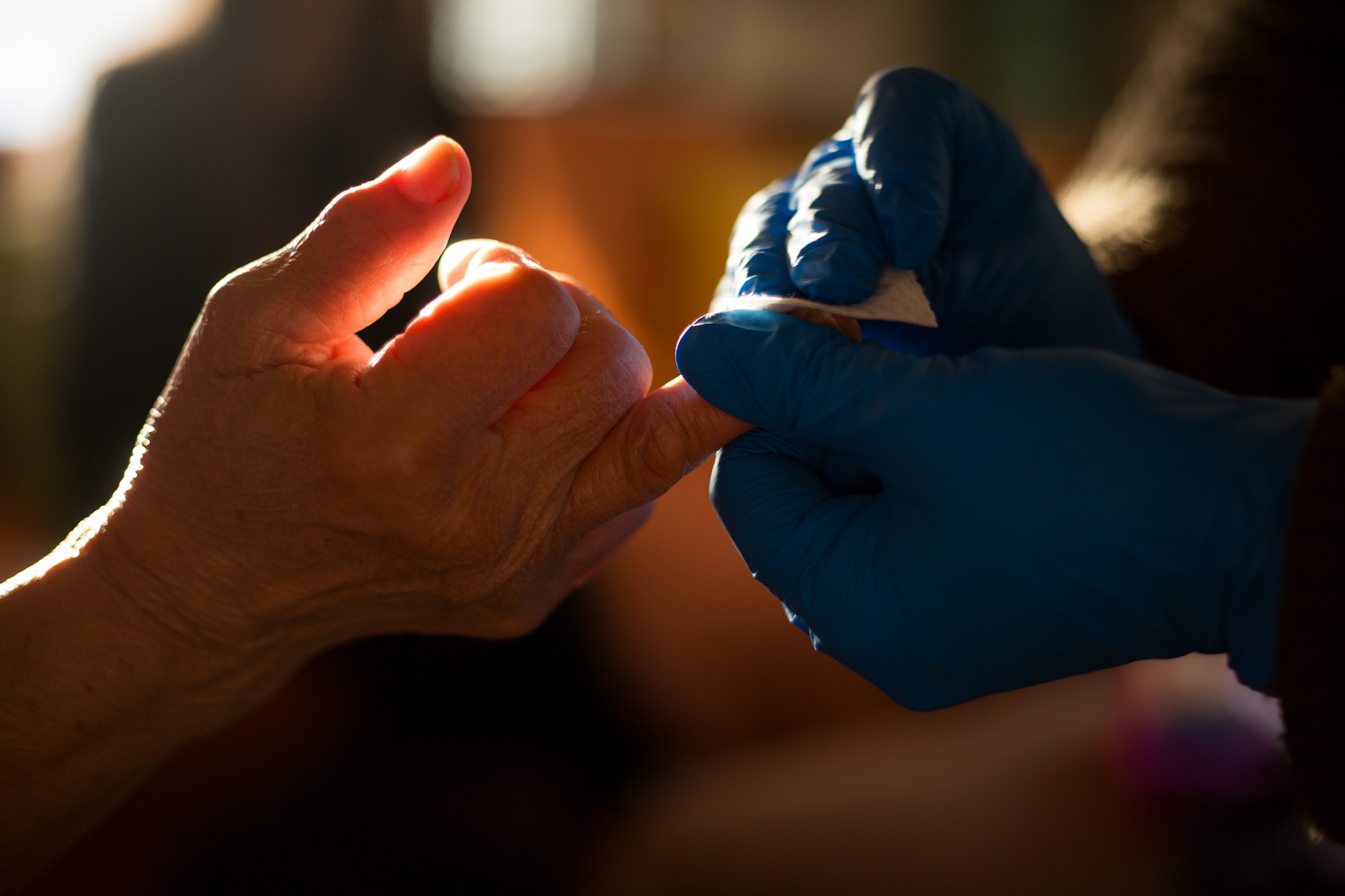
Upon her enrollment, community health worker Fanny Ochoa conducted an initial assessment that moved beyond clinical vitals. Ochoa identified that Charmaine’s physical health was inextricably linked to her housing situation and her mental well-being. Over the course of the following year, the two worked as a team. Ochoa facilitated Charmaine’s move into Oliver Station—a modern, affordable housing development in Camden created by the Michaels Organization and Virtua Health—which features on-site primary care.
Furthermore, the program integrated advanced medical technology into Charmaine’s daily routine. She was provided with a wearable continuous glucose monitor (CGM), allowing for real-time tracking of her blood sugar levels. This combination of stable housing, emotional support, and technological monitoring led to a total stabilization of her COPD and diabetes.
Bridging the Gap: The Role of Community Health Workers
Community health workers serve as the "connective tissue" between the healthcare system and the community. Workers like La Shawn Dutton-Spruill are trained to navigate the complex web of social services that patients often find overwhelming. Dutton-Spruill’s work with a patient named Denise highlights the program’s ability to rescue individuals from the "cracks" of the traditional system.
When Dutton-Spruill first met Denise, the patient was living in a condemned structure, missing medical appointments, and failing to take prescribed medications for her hypertension. The intervention began with bi-weekly check-ins to establish trust. Once a rapport was built, the team addressed Denise’s immediate need for safe housing and nutrition.
Access to healthy food is a cornerstone of the Healthy Neighbor initiative. Through Virtua Health’s "Eat Well" program, participants are connected to mobile grocery markets that deliver fresh produce to underserved neighborhoods. Patients can utilize "food bucks" provided by the program, alongside federal Supplemental Nutrition Assistance Program (SNAP) benefits, to purchase high-quality groceries. For Denise, the shift from a state of crisis to stability resulted in a dramatic improvement in her mental health and clinical indicators.

Clinical Data and Program Efficacy
The anecdotal success of the Healthy Neighbor program is backed by significant clinical data. According to recent reports from Virtua Health:
- Hypertension Control: 74 percent of participants who entered the program with uncontrolled hypertension saw a meaningful and sustained improvement in their blood pressure levels.
- Diabetes Management: Nearly 70 percent of patients with Type 2 diabetes experienced a significant reduction in their HbA1c (blood sugar) levels.
- Sustainability: By addressing the root causes of health instability—such as housing and food access—the program ensures that clinical improvements are maintained long after the 12-month intervention period concludes.
These figures suggest that the "whole-person" approach is more effective than traditional outpatient care for populations facing high levels of social stress. By mitigating the "noise" of poverty, the program allows clinical treatments to finally take hold.
Chronology of Expansion and the National Toolkit
The Healthy Neighbor program has evolved from a local pilot into a scalable model for national healthcare reform.
- Initial Launch: The program began as a partnership between Virtua Health and Medtronic LABS, focusing on the specific needs of Camden’s most vulnerable populations.
- Expansion Phase: Following early success, the city of Camden provided a dedicated grant to expand the community health worker team, allowing the program to reach a larger volume of patients.
- August 2025: Virtua Health and Medtronic LABS officially released a comprehensive toolkit titled "The Healthy Neighbor Model: A Guide for Health Systems." This open-source document provides a blueprint for other hospitals and healthcare providers to replicate the Camden success story.
- Current Status: Plans are currently underway to expand the program’s footprint beyond Camden into other regions of New Jersey and potentially nationwide.
Daniel Master, director of community health and impact at Virtua Health, emphasizes that the goal is to open-source the initiative’s successes. "We want to share this because we know what we’re doing is unique," Master stated. "We are proving that addressing social determinants is not just a moral imperative, but a clinical necessity."
Economic Challenges and the Path to Sustainability
Despite the clear clinical and social benefits, the Healthy Neighbor model faces significant structural hurdles, primarily regarding long-term funding. In the current U.S. healthcare landscape, most private and public insurers do not have a reliable reimbursement mechanism for the services provided by community health workers. While insurance companies typically pay for medications, surgeries, and nutrition consultations, the "boots-on-the-ground" work of navigating a patient through a housing application or conducting home visits is often not covered.

This lack of a reimbursement framework forces programs like Healthy Neighbor to rely on grants, philanthropic donations, and the internal budgets of large health systems. Analysts suggest that for this model to become a standard of care, federal and state policy changes are required to recognize CHWs as essential medical providers.
Furthermore, there is a general lack of awareness within the broader medical community regarding the depth of the CHW role. While many systems utilize "patient navigators," the Healthy Neighbor approach is distinct in its intensity and its focus on the home environment over the clinic environment.
Analysis: A Paradigm Shift in American Healthcare
The success of the Healthy Neighbor program in Camden represents a broader shift in American healthcare from "volume-based" care to "value-based" care. In a volume-based system, providers are paid for the number of tests and procedures they perform. In a value-based system, the focus is on the patient’s overall health outcome.
The Camden model argues that it is more cost-effective for a health system to invest in a year of community health worker visits and fresh produce than to pay for a single, multi-day hospital stay resulting from a diabetic coma or a stroke. By preventing the crisis before it occurs, the program potentially saves the healthcare system millions of dollars in emergency room costs and intensive care treatments.
Moreover, the partnership between a healthcare provider (Virtua), a technology giant (Medtronic), and the social service sector (The Michaels Organization) provides a template for "cross-sector collaboration." This multi-disciplinary approach acknowledges that the medical community cannot solve the health crisis in isolation; it requires the active participation of urban planners, food distributors, and government agencies.

Future Outlook
As Virtua Health and Medtronic LABS look toward the future, the focus remains on the sustainability of the intervention. The 12-month limit on the program is designed to empower patients with the tools they need to manage their own health independently. However, the program’s leaders acknowledge that as long as poverty and housing shortages persist, the need for such interventions will remain.
The Healthy Neighbor initiative has proven that even in cities with profound historical disadvantages, significant health improvements are possible when the system meets the patient where they are. For residents like Charmaine and Denise, the program did more than just lower their blood pressure; it provided them with the stability and dignity required to live their lives to the fullest. As the model gains national attention, it may well serve as the foundation for a more equitable and effective American healthcare system.






